Six months on since the first cases of COVID-19 emerged in Wuhan, many of us in the UK will be feeling a mix of relief and trepidation as the national lockdown eases. The loosening of restrictions will allow us to see friends and family (albeit still at a distance) and plan a return to a more normal life. With warmer weather, these changes have brought hope.
In the UK, where the Prime Minister is one of the higher-profile of the world’s now more than 10 million COVID-19 cases, the government is understandably anxious to get society and the economy back on track. This is what we all want: indeed, it’s what scientists are striving to ensure.
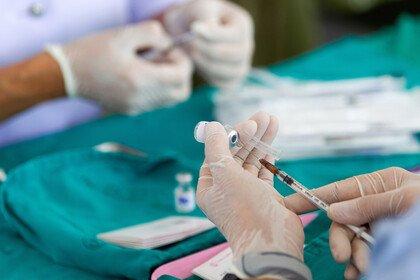
Since the virus began to ripple across the world, scientists have worked at incredible speed to increase understanding of COVID-19. In record time there have been incredible advances, with over 200 vaccine candidates already in development and a treatment, dexamethasone, that we now know saves lives. We’ve achieved in months what would normally take decades.
But these huge leaps must not lull us into a false sense of security. Though national lockdowns have saved many lives, the virus hasn’t gone away. The road to eliminating COVID-19 still contains many unknowns. We don’t yet know how the virus will evolve, how immunity is generated or how long it lasts. We don’t have a vaccine to stop people getting sick, or a range of different treatments to help them avoid the need for hospitalisation or getting worse, if already in hospital.
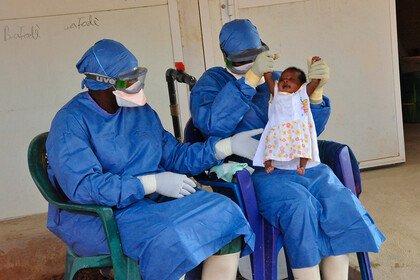
Globally, the pandemic is accelerating and spreading into new areas of the USA, Central South America, South Asia and Africa. Over 10 million cases and 500,000 deaths, both undoubtedly underestimates, are grim milestones a long way from any final tolls.
Countries that have managed to reduce cases and can now start to cautiously ease lockdowns remain at risk of rebounds and further waves. In places such as Beijing, North Rhine-Westphalia, and here in Leicester, there have recently been worrying increase in number of new cases. The USA is still seeing a daily increase in cases, over six months since the first patient was identified. The situation in the UK and USA, two countries who have suffered disproportionately, balances on a knife edge.
Across Europe, and in the UK in particular, governments must take the time to step back, be critical and honest, and learn from the experiences of the last six months to avoid further crisis and cope with a potential second wave, which we have to assume and prepare for in the winter.
Having robust testing, tracing and isolating systems is vital – with testing in the community, hospitals, care homes, schools. Data must be shared rapidly with relevant public health authorities and communicated with local communities. Having the data is not enough. It must lead to rapid action, actions that are pre-planned, well communicated, trusted, locally-led and focused.
Robust systems for testing, tracing and isolating potential coronavirus cases are essential components to controlling the pandemic. But these aren’t the long-term solutions that are needed. Securing effective vaccines, treatments and diagnostics for COVID-19, and strengthening public health are the only ways to bring this pandemic to an end, preventing future tragedies and returning the world to some secure sense of normality.
Until every country is protected, we all remain at risk from coronavirus. This disease pays no attention to national borders. We will need billions of doses for vaccines and treatments. Nothing on this scale has ever been attempted before, and current manufacturing and distribution capacity is nowhere near enough to deliver such a feat.
It will also not come cheap. The World Health Organization and partners of the ACT-Accelerator, a global collaboration to share the costs and the risks of backing a large number of vaccine and treatment candidates, have now set the total cost of this effort at $31.3 billion. To date, $3.4 billion has been raised.
I’ve been impressed over the last few months by the unprecedented levels of support from governments, industry and philanthropy for science, and unprecedented global collaboration. It’s what has made the remarkable scientific progress so far possible. Attempts by nations to buy-up stocks of treatments and vaccines, or potential products, to only protect their own citizens is not just wrong on moral and ethical grounds, it is also not smart public health. Infectious disease does not respect borders.
A huge amount of money is still required, and $3.4 billion is a tiny fraction compared to the ongoing human and economic cost of COVID-19. This crisis could cost the global economy $12 trillion, according to the International Monetary Fund. By coming together through the ACT-Accelerator, countries will have a greater chance of securing treatments for their citizens.
Securing equitable access to vaccines, treatments and tests for all is not altruism: it is in every country’s best interest to work together to prevent second waves and avoid many more years of preventable deaths and economic hardship. Leaving countries behind would jeopardise the entire endeavour – with ramifications felt among both high- and low-income countries alike.
In the past six months, we have learned a huge amount about coronavirus. We are better at treating it and mortality rates have come down, but there is no getting around the enormity of the task ahead of us. The longer we wait, the worse the damage will be. We are still at the start of this pandemic and there is only one exit strategy – interventions that change the fundamentals of infection, transmission and illness.
We must learn from the first six months, redouble our efforts, and we must continue to act together. The way countries work together on COVID19, or not, will define their relationships for decades to come.
A version of this article was first published in The Guardian.